Pemphigoid Case Study
Pemphigoid
Group of rare autoimmune blistering skin diseases. As its name indicates, pemphigoid is similar in general appearance to pemphigus, but pemphigoid does not feature acantholysis, a loss of connections between skin cells.
It can be divided into:
BULLOUS PEMPHIGOID OR MUCOUS MEMBRANE (CICATRICIAL) PEMPHIGOID BULLOUS PEMPHIGOID
![]()
It is a chronic, inflammatory, subepidermal, blistering disease. If untreated, it can persist for months or years, with periods of spontaneous remissions and exacerbations. The disease can be fatal, particularly in patients who are debilitated.
Pemphigoid is more common than pemphigus, and is slightly more common in women than in men. It is also more common in people over 60 years of age than it is in younger people.
It is more prevalent in elderly patients with neurological disease, particularly stroke, dementia and Parkinson disease. A drug, an injury, or skin infection can also trigger the onset of disease.
SIGNS AND SYMPTOMS
Bullous pemphigoid may present with several distinct clinical presentations, as follows:
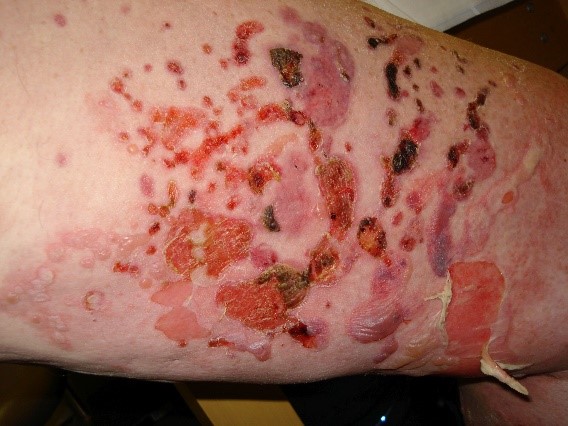
Generalized bullous form: The most common presentation; tense bullae arise on any part of the skin surface, with a predilection for the flexural areas of the skin
Vesicular form: Less common than the generalized bullous type; manifests as groups of small, tense blisters, often on an urticarial or erythematous base
Urticarial form: Some patients with bullous pemphigoid initially present with persistent urticarial lesions that subsequently convert to bullous eruptions; in some patients, urticarial lesions are the sole manifestations of the disease
CASE STUDY EXAMPLES
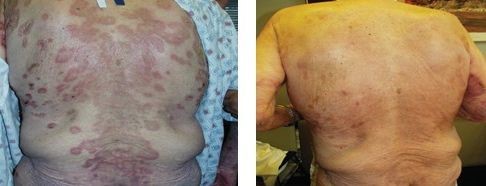
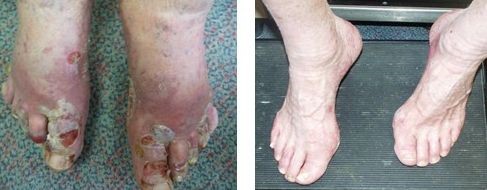
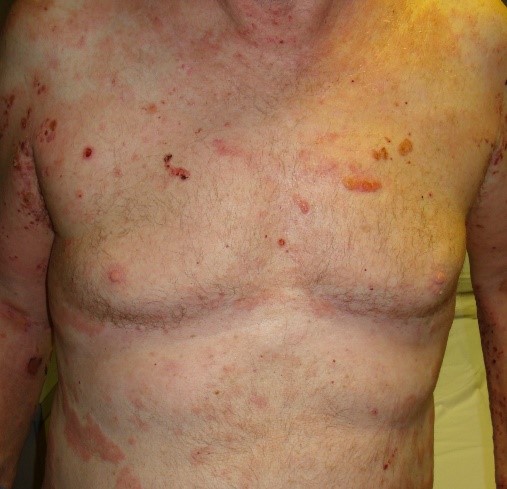
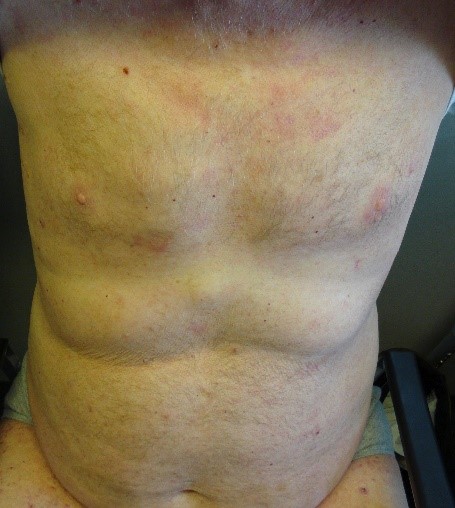
MUCOUS MEMBRANE (CICATRICIAL) PEMPHIGOID
![]()
A rare chronic autoimmune subepithelial blistering disease characterized by erosive skin lesions of the mucous membranes and skin that results in scarring of at least some sites of involvement. Blistering lesions can also be found on the face, neck and scalp.
The autoimmune reaction most commonly affects the mouth, causing lesions in the gingiva or gums, but it can also affect areas of mucous membrane elsewhere in the body, such as the sinuses, genitals and anus. When the cornea of the eye is affected, repeated scarring may result in blindness.
SIGNS AND SYMPTOMS
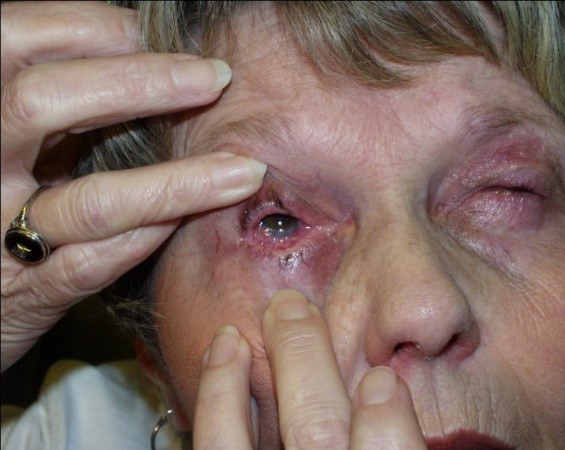
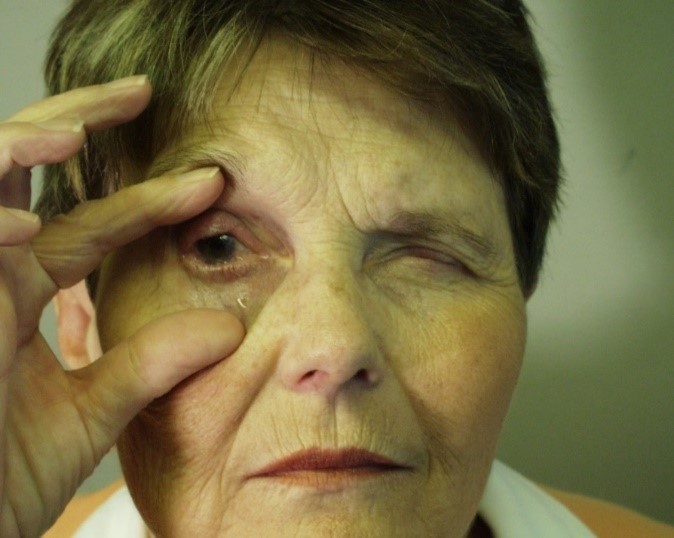
Eye
- Sensation of grittiness or pain
- Conjunctivitis
- Lesions form, erode and heal to leave scar tissue
- May lead to impaired vision or blindness
Mouth
- Blisters form first on the gums near the teeth
- Palate, tongue, lips, buccal mucosa, floor of the mouth and throat may be affected
- Painful erosions and ulcers make it difficult to eat
- Weight loss and nutritional deficiencies may develop due to starvation
- Lesions occurring in the throat (oesophagus, trachea and larynx) can become life-threatening
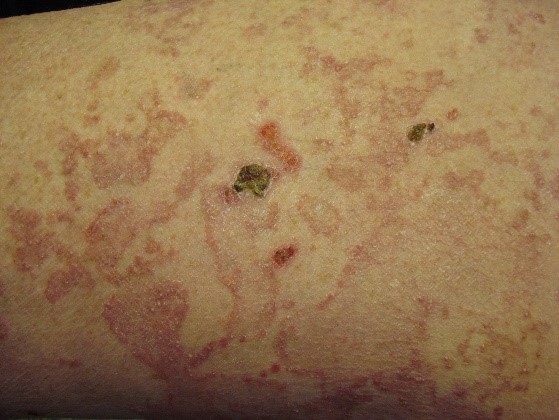
Skin
- Blisters on the skin develop in 25–30% of patients
- May be itchy
- Bleeding may occur if traumatised
Genitals
- Painful blisters, erosions and swelling of the clitoris, labia, and anus in women, and of the penis and anus in males
- Scarring can lead to severe distortion of genitalia
- May cause difficulty and pain passing urine
- Adhesions can lead to narrowing or even closure of the vaginal orifice
DIAGNOSIS
To establish a diagnosis of bullous pemphigoid, the following tests should be performed: histopathologic analysis from the edge of a blister and DIF studies on normal-appearing perilesional skin.
If the DIF result is positive, indirect immunofluorescence (IDIF) is performed using the patient’s serum. The preferred substrate for IDIF is salt-split normal human skin substrate.
TREATMENT
The primary aim of treatment is to stop blister formation, promote healing and prevent scarring. Mucous membrane pemphigoid is a particularly difficult disease to treat as it can affect so many different parts of the body. Usually a team of medical specialists are required for overall care. Regular examinations are necessary.
The most common treatment is the administration of oral steroids, especially prednisone, often in high doses.
The side effects of corticosteroids may require the use of so-called steroid-sparing or adjuvant drugs. Various immunosuppressant treatments are available.
However, long term use of either prednisone or immunosuppressive agents can lead to harmful and sometimes fatal side effects.
Intravenous gamma globulin (IVIG) has been proven to be useful in severe cases. Recently, Rituximab, an anti-CD20 antibody, was found to improve otherwise untreatable severe cases of Pemphigoid
Research
Foster CS, Chang PY, Ahmed AR. Combination of rituximab and intravenous immunoglobulin for recalcitrant ocular cicatricial pemphigoid: a preliminary report. Ophthalmology. 2010 May;117(5):861-9.
Shetty S, Ahmed AR. Critical analysis of the use of rituximab in mucous membrane pemphigoid: a review of the literature. J Am Acad Dermatol. 2013 Mar;68(3):499-506.
Ahmed AR, Shetty S, Kaveri S, Spigelman ZS. Treatment of recalcitrant bullous pemphigoid (BP) with a novel protocol: A retrospective study with a 6-year follow-up. J Am Acad Dermatol. 2016 Apr;74(4):700-708.e3.
